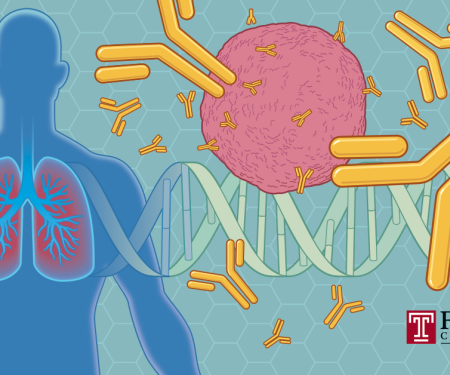
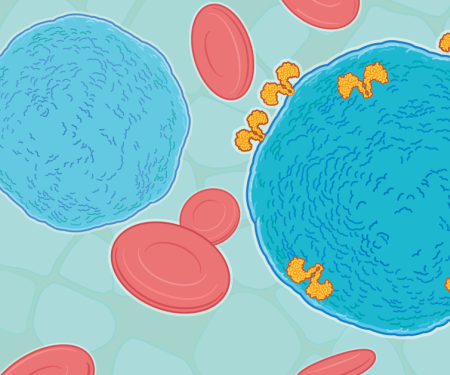
Immunotherapy uses the body’s own immune system to fight cancer. The immune system is made up of different kinds of cells that patrol the bloodstream for intruders and abnormal cells like cancer. These immune cells can be trained to recognize and fight cancer. Researchers and physicians at Fox Chase Cancer Center are at the forefront of expanding how this exciting new therapy can treat cancer.
How Immunotherapy Works
The immune system naturally scans the body for cancers and is usually effective in killing cancerous cells. However, sometimes a tumor finds ways to avoid immune cells, allowing it to grow and spread, undisturbed by the immune response. If the immune system can be trained or re-focused to recognize and attack a cancer, it can adapt along with the cancer and maintain a longer-term response. That’s what immunotherapy does.
Today, Fox Chase is committed to the clinical development of immunotherapy. Our researchers will help discover which patients have the “markers” to benefit from treatment, how immunotherapy can be combined with chemotherapy, targeted therapy, and radiation for more effective cancer eradication, and whether the approaches can be used not only to treat cancer after it has spread, but also to prevent cancer recurrence.
Types of Immunotherapy Offered at Fox Chase
Checkpoint Inhibitors
Checkpoint inhibitors empower the patient’s own immune cells to recognize and attack tumors. The immune system keeps immune T cells from accidentally attacking healthy cells. Cancer cells can take advantage of this by disguising themselves as normal cells. Checkpoint inhibitors disrupt this disguise, unleashing the T cells on cancer.
CAR T-Cell Therapy
Chimeric antigen receptor (CAR) T-cell therapy uses a patient’s own T cells to destroy cancer cells. Scientists take T cells from a patient’s blood, modify them so that they recognize cancer, and then infuse these cancer-fighting T cells back into the patient.
Oncolytic Viruses
Oncolytic viruses selectively infect and kill cancer cells. To create this therapy, existing viruses are modified in the lab so they selectively destroy cancer cells without affecting normal cells. Modified virus can be injected directly into a melanoma tumor, for example. The virus multiplies, causing cancer cells to rupture and die. Once the cells explode, antibodies are released that help mount an immune response.
Vaccines
Cancer treatment vaccines are designed to get the immune system to attack abnormal cells, including cancer cells. One vaccine is approved in the U.S. for treatment-resistant advanced prostate cancer, and many others are being studied. Similar to CAR T-cell therapy, immune cells are removed from the patient, enhanced, and returned to the patient.
Monoclonal Antibody Therapy
The immune system makes a protein called an antibody to help fight infection. Antibodies circulate throughout the body and hunt for foreign substances to destroy. Monoclonal antibodies (mAbs) are molecules produced in a lab, and are engineered to mimic or enhance the way the body’s immune system kills cancer. Depending on the therapy, mAbs can detect and attach to cancer cells, sending a signal other immune system cells about the cancer’s location. They can also trigger an immune system response to swarm and destroy cancer cells.
“Fox Chase Cancer Center has really been a major figure in the development of immunotherapy. One of our early trials led to approval of one of the immunotherapy drugs. Today, we have multiple researchers asking us to run their trials for new immunotherapy drugs. There’s a real depth of leadership and experience in this area, and a commitment to further studies.” — Joseph Treat, MD, lung cancer specialist