Related Articles
00 / 00

Request an Appointment
Chair, Department of Radiation Oncology, Lewis Katz School of Medicine at Temple University
Chair, Department of Radiation Oncology, Fox Chase Cancer Center
Professor
Gerald E. Hanks Endowed Chair in Radiation Oncology
NCCN, Prostate Cancer Panel Member
Urethral Cancer, Penile Cancer, Ureteral Cancer, Kidney Cancer, Testicular Cancer, Bladder Cancer, Prostate Cancer
In addition to my focus on treating and caring for patients with prostate and bladder cancer, it is my responsibility as Chairman of the Department of Radiation Oncology at Fox Chase; an NCI designated National Comprehensive Cancer Center to promote the mission of the Center to prevail over cancer. Our department's expertise has always focused on developing and integrating sophisticated technology into successful treatment for our cancer patients and I remain committed to continuing and expanding this legacy. However, the successful treatment of a patient is not just based on the technology that is available. Being diagnosed with cancer and receiving treatment is one of the most difficult things that many people will ever face, and it is crucial that we as caregivers do not forget this. Caring for patients as one important part of a multidisciplinary team allows us in the Department of Radiation Oncology to provide the best possible care for our patients.
The mission of Fox Chase Cancer Center Radiation Oncology is to alleviate the burden of cancer by safely and compassionately delivering state-of-the-art radiation therapy with a commitment to clinical excellence, research expertise, and education in an inclusive environment that embraces diversity.
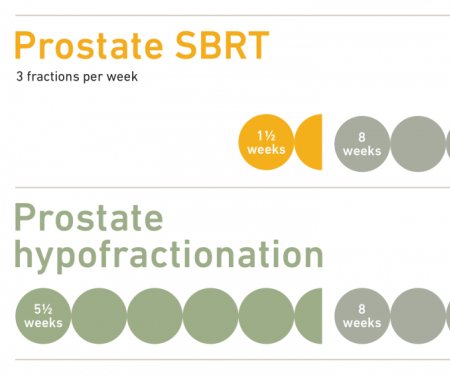
The Department of Radiation Oncology at Fox Chase Cancer Center and the Lewis Katz School of Medicine at Temple University offer many of the most sophisticated radiation techniques, including adaptive radiation therapy, hypofractionated intensity modulated radiation therapy (IMRT), stereotactic radiosurgery (SRS), stereotactic body radiation therapy (SbRT), high-dose-rate (HDR) brachytherapy, and the GammaKnife radiosurgery system. We have some of the most extensive experience in adaptive radiation therapy and HDR brachytherapy in the region and country.
But we believe caring for people with cancer is more than just a collection of technologies. Although crucial to delivering state-of-the-art treatment, advanced technologies are just one component of what we have to offer our patients. As part of a National Cancer Institute-designated Comprehensive Cancer Center, we believe that cancer care is truly multidisciplinary, so we work with our Fox Chase colleagues, many of whom are national and international experts in surgical and medical oncology. This level of expertise and care offers our patients the best opportunity for treatment success.
The Fox Chase Department of Radiation Oncology is one department located at four sites in Northeast Philadelphia, Bucks County, Montgomery County, and North Philadelphia. This gives cancer patients in Southeastern Pennsylvania, New Jersey, and Delaware access to Fox Chase Radiation Oncology regardless of location.
In addition to providing state-of-the-art care, Fox Chase radiation oncologists are involved in developing new treatments through research. The foundation of modern cancer care rests on clinical, basic science, and translational research. We have a decades-long history of developing many of the treatments that are now standard, including 3D conformal radiation therapy, IMRT, and image-guided radiation therapy. We are a department of firsts, including the first CT simulator (1989) and the first MRI simulator (2000) in the United States. The first temporary HDR prostate implant on the East Coast was performed at Fox Chase in 1998, and now we are the first and only department in the United States developing and treating patients with radiodynamic therapy.
Fox Chase Radiation Oncology is also looking to the future, as evidenced by its commitment to train the next generation of radiation oncologists, medical physicists, and radiation therapists. We have been training radiation oncologists in our residency program for more than 40 years and we remain a top choice for elite medical students from around the country. Education is a priority for the radiation oncology and medical physics faculty, and preparing the next generation of clinicians and physicists is one of our key missions.
Through clinical excellence, research innovation, and educational distinction, Fox Chase Radiation Oncology offers the highest level of care for our patients in their time of need.
In the early 2000s I was a real estate agent living and working in Ocean County, New Jersey.

My decades-long career working for companies involved in the healthcare industry took me all over the United States, from the Northeast, to the Midwest, to the South. Years later, so did my cancer treatment, eventually leading me at Fox Chase Cancer Center.

I’ve been a tennis coach for nearly 17 years, the last dozen at Legacy Youth Tennis and Education in Philadelphia. I run group clinics and offer private lessons. I specialize in movement and footwork training, as well as video-based training. My students range from kids as young as five to professional tennis players. I’m an active coach. When I teach my students how to do something, I want to show them I can do it. They’re amazed at how good I am!

I’m 66 years old and a resident of Princeton, New Jersey. I’m retired now, but I worked on Wall Street for 43 years and have been looking forward to spending my retirement doing things I love like playing golf, running, and giving back to the community.
Horwitz, E.M.; Bae, K.; Hanks, G.E.; Porter, A.; Grignon, D.; Brereton, H.; Venkatesan, V.; Lawton, C.A.; Rosenthal, S.A.; Sandler, H.M.; Shipley, W.U. Ten-Year Follow-Up of RTOG 92-02: A Phase III Trial of the Duration of Elective Androgen Deprivation in Locally Advanced Prostate Cancer. Journal of Clinical Oncology 26: 2497-2504; 2008. PubMed
Langer, C.J.; Harris, J.; Horwitz, E.M.; Nicolaou, N.; Kies, M.; Curran, W.J.; Wong, S.J.; Ang, K.K. Phase II study of paclitaxel, cisplatin in combination with split course concomitant hyperfractionated re-irradiation in patients with recurrent squamous cell cancer of the head and neck cancer: Preliminary results of RTOG 99-11. Journal of Clinical Oncology 25: 4800-4805; 2007. PubMed
Horwitz, E.M.; Levy, L.B.; Thames, H.D.; Kuban, D.A.; Kupelian, P.A.; Martinez, A.A.; Michalski, J.M.; Pisansky T.M.; Sandler, H.M.; Shipley, W.U.; Zelefsky, M.J.; Hanks, G.E.; Zietman, A.L. The Biochemical And Clinical Significance Of The Post-Treatment PSA Bounce For Prostate Cancer Patients Treated With External Beam Radiation Therapy Alone: A Multi-Institutional Pooled Analysis. Cancer 1071: 1496-1502; 2006. PubMed
Kuban, D.A.; Levy, L.B.; Potters, L.; Beyer, D.C.; Blasko, J.C.; Moran, B.J.; Ciezki, J.P.; Zietman, A.L.; Zelefsky, M.J.; Pisansky, T.M.; Elshaikh, M.; Horwitz, E.M. Comparison of biochemical failure definitions for permanent prostate brachytherapy. International Journal of Radiation Oncology Biology and Physics 65: 1487-1493; 2006. PubMed
Horwitz, E.M.; Thames, H.D.; Kuban, D.A.; Levy, L.B.; Kupelian, P.A.; Martinez, A.A.; Michalski, J.M.; Pisansky T.M.; Sandler, H.M.; Shipley, W.U.; Zelefsky, M.J.; Hanks, G.E.; Zietman, A.L. Definitions Of Biochemical Failure That Best Predict Clinical Failure In Prostate Cancer Patients Treated With External Beam Radiation Alone - A Multi-Institutional Pooled Analysis. Journal of Urology 173:797-802; 2005. PubMed
Horwitz, E.M.; Uzzo, R.G.; Hanlon, A.L.; Greenberg, R.E.; Hanks, G.E.; Pollack, A. Modifying the ASTRO definition of biochemical failure to minimize the influence of backdating in patients with prostate cancer treated with 3D conformal radiation therapy alone. Journal of Urology 169: 2153-2159; 2003. PubMed
Hanks, G.E.; Hanlon, A.L.; Epstein, B.; Horwitz, E.M. Dose response in prostate cancer with 8-12 year follow-up. International Journal of Radiation Oncology Biology and Physics 54: 427-435; 2002. PubMed Collapse
The following ratings and reviews are based on verified feedback collected from independently administered patient experience surveys. The ratings and comments submitted by patients reflect their own views and opinions. Patient identities are withheld to ensure confidentiality and privacy. Learn more about our Patient Experience Ratings.






























Patient comments
Excellent team
Professional and courteous!
Can't say enough positives about Dr. Horwitz--extremely knowledgeable, compassionate and most importantly, down-to-earth and easy to talk to.
Outstanding discussion with Dr Horwitz
Dr was exc!