Ethics of the Fathers
“Whoever saves a life, it is as if he saved an entire world.” —Mishnah Sanhedrin 4:5

"But what is the most effective way to teach our fellows the ethical conduct of research?" As if a subliminal alarm clock had just sounded, I awoke with a start. I was attending a national conference on research ethics, my interest spurred by my dual role at the time as chairman of the hospital institutional review board and director of the pulmonary fellowship training program. However, when the discussion veered to the moral and regulatory nuances of competence, equipoise, and substituted judgment, mental exhaustion gained the upper hand. Dozing intermittently on the last conference day, I briefly rallied for this final discussion, yet like many verbal exchanges among intelligent, impassioned experts, the debate yielded more questions than answers. The meeting adjourned, and I welcomed the transition from the chilly conference room to the warm autumn sunshine as I stepped outside in our nation’s capital.
With several hours before my evening train home and nowhere special to go, I wandered across the mall and soon found myself at the entrance to the United States Holocaust Memorial Museum. In the 10 years since it had opened, I had hoped to visit but not yet had the chance. Without children in tow or a pressing agenda at hand, I knew the present opportunity would not come again soon. I stepped inside.
The museum exhibit was arranged chronologically, carefully cataloging the persecution and destruction of Europe’s unwanted peoples—Jews, homosexuals, Roma, the mentally infirm. To walk attentively from room to room was to witness genocide unfold in slow motion; rants transitioning to goosesteps, smashed windows into shattered lives. Viewing the collection was like watching freezeframe video of a seismic eruption. One intuitively understood that a cataclysmic destruction was at hand but was helpless to intervene or refrain from watching. The most graphic images appeared toward the end of the exhibit.

In one of the final rooms was a photographic display at floor level, surrounded by a 4-foot barrier. As I approached the low wall, I looked over to see the distorted faces of camp inmates who were the subjects of brutal experimentation. Concentration camp physicians had exposed prisoners to extremes of water temperature and barometric pressure to determine human tolerance to the elements that might be encountered by pilots forced to ditch their aircraft. I assumed that the barrier was intended to limit young children from seeing the anguish of the victims. Silently, I wondered which was the greater concern of the museum personnel: traumatizing children with images of physical torture or traumatizing them with the knowledge that physicians were willing participants in inflicting such torture.
I learned from the museum that law enforcement personnel visited the exhibits on special tours, to understand the potential for abuse that accompanies power. In recalling the morning’s unresolved question, I realized that physician-trainees could benefit from a similar program. One visit here would probably provide a more lasting lesson on the necessary boundaries of scientific inquiry than a series of classroom lectures on medical ethics. Of course, it was hardly practical to bring our fellows to Washington, DC, to calibrate their moral compass. Perhaps there was another way.
A few weeks later, I prepared for our Friday morning conference on chest imaging. The goal of the conference was to present unknown films with limited clinical information, to teach fellows to form a differential diagnosis based on the radiographic findings alone. I pulled a specific set of images and headed to the conference room. As the session started, I placed a chest x-ray on the viewbox.
“What do you see?” I asked. “A left upper lobe lung nodule,” came the reply. Clearly, there was a sharply circumscribed opaque shadow— an obvious white oval within the darkened lung field.
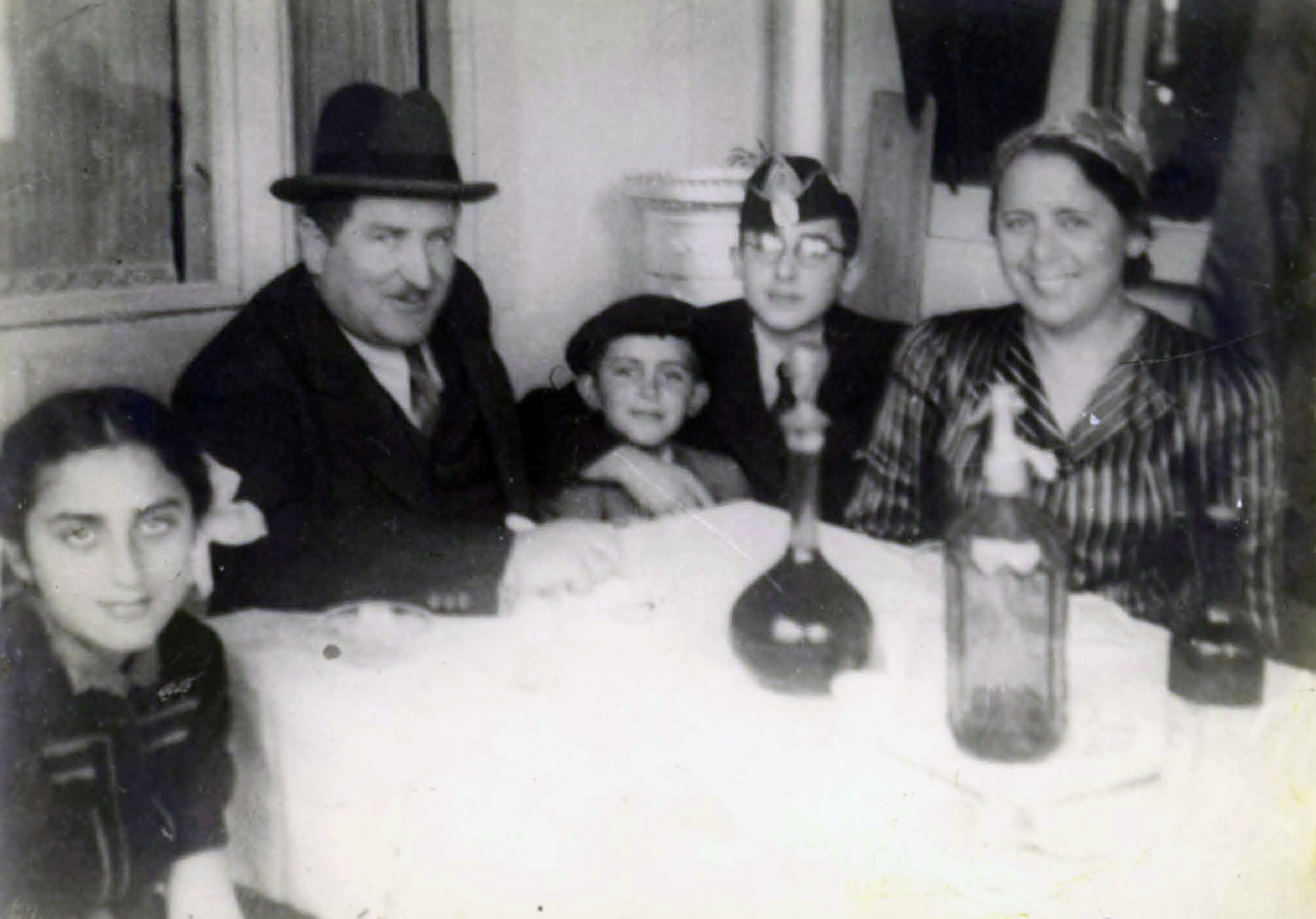
“And on the lateral?” I continued. Despite intense scrutiny, a nodule could not be seen. “Can we see a CT?” the fellows asked. I provided CT images of the chest. The “lung nodule” was now visible as a calcified pleural plaque, not a nodule at all. I highlighted the intended lesson: A 2-dimensional image does not always accurately portray 3-dimensional reality. Sometimes one has to look deeper.
Customarily, we moved rapidly through films in this conference, but instead of showing the next case, I digressed to provide background on the patient of this particular radiograph. As a 17-year-old teenager, this young man and his father were imprisoned in a Nazi labor camp during World War II. In the winter of 1944, the teenager developed pleurisy, fever, anorexia, and weight loss. Unable to work, he was brought to the infirmary. The camp physician improvised a drainage system for the effusion, offered the meager services available at the time to assist a Jewish inmate, and turned his attention to other matters. Returned to the barracks and expected to work, the young man stood little chance of surviving the elements.
To even the odds, his father implored a fellow inmate—a dentist when one’s profession mattered—to pry the father’s gold crowns from his teeth for use as currency. The dentist complied, using the crude utensils available in camp, and the painfully extracted bribe was offered to the barracks guard. A few grams of gold netted several weeks of barracks restriction for the teenage son—enough time to regain the strength needed to endure the rigors of camp life. Even considering that life in a labor camp had little value, this was a bargain price, readily paid by the father, to ensure his son’s survival. Father and son were liberated the following spring, and the films were obtained years later as part of a preoperative pulmonary assessment.
We digressed further and discussed the actions of the camp doctor and their ethical ramifications. Did a physician’s obligations to a prisoner differ from his responsibilities to a non-inmate patient when resources were scarce? If a physician modified a procedure to provide treatment, was this medical care or experimentation? At a time of medical privation, was it ethical to render acute treatment but insufficient after-care? And a final, broader question: How could one ensure that external societal forces would not corrupt a physician’s moral judgment? This last question proved the thorniest to answer.
As the discussion continued, a parallel story occupied my thoughts. About 500 km to the east, at around the same time, a 14-year-old girl was having a very different encounter with a very different Nazi physician: selection day. As she gathered the courage to walk past a review platform with her fellow inmates, she rotated her torso laterally so that the inspecting physician would not see the inflamed and excoriated insect bites and sores on her back. The subtle feint was skillfully executed, and the doctor triaged her to the right—to survival. The girl’s mother had not been so lucky. With an indifferent wave of the hand that belied the magnitude of the summary judgment, the camp physician dispatched her to the left when she first arrived at Auschwitz. Her first day at the camp was her last.

In cancer research, much effort has been expended to understand the signals and pathways that turn a cell malignant. But how does one explain the physician who has become malignant? Here were two men, steeped in the same medical tradition, subject to the same propaganda, and caught within the same political and military system. Yet while one retained a measure of human compassion and personal ethics, the other was bereft of both. The medical profession is not a job; it is not even a calling. It is a gift we are given, to touch another’s life in awesome and profound ways. We discard this gift at our own peril. Primum non nocere, our medical forefathers advised. First, do no harm. Once we cross this boundary, all is lost.
The radiology conference ended. I left with a sensation reminiscent of that autumn afternoon in Washington, warmed not by a gentle breeze but from the knowledge that a chest x-ray teaching session could provide something more than simply a lesson in radiology. Of the questions I had anticipated, one remained unasked: How do you know so much about the background of this patient?
I had rehearsed my answer. “From stories told to me, when I reached an age of remembrance and understanding,” I envisioned replying, “of my father’s pleurisy, my mother’s back, and my grandfather’s gold teeth.”
* - perished in the Holocaust.
