Has Robotic Cystectomy Reached the Mainstream?
-
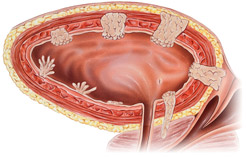
The current gold standard therapy for muscle invasive bladder cancer consists of a combination of systemic chemotherapy and surgical resection. Radical cystoprostatectomy (removal of the bladder and prostate) in men, and anterior pelvic exenteration (removal of the bladder, uterus, ovaries and a portion of the vagina) in women, in combination with removal of the regional lymph nodes, has long been the preferred surgical procedure to maximize local control of disease and prolong survival.
Due to the technically challenging nature of the surgery, including urinary tract reconstruction and nerve preservation, removal of the bladder has traditionally been performed via an open approach, through an incision stretching from the belly button to the pubis. However, as the experience with minimally invasive (laparoscopic and robotic) urologic procedures such as prostatectomy and partial nephrectomy has grown, surgeons have become increasingly confident that robotic cystectomy is a feasible and often preferred surgical approach in the management of bladder cancer.
Two recent studies (listed below) have confirmed what most urologic oncologists with significant minimally invasive training have long suspected:
- Robotic cystectomy affords the traditional advantages as other minimally invasive procedures, with equivalent oncologic efficacy.
- Robotic surgery offers enhanced visualization and improved precision, which results in less blood loss and facilitates neurovascular bundle preservation and lymph node dissection.
- Smaller, less painful incisions aid in a shortened hospital length of stay and quicker post operative recovery.
It is important to realize that surgical approach should not impact the decision to perform a continent urinary diversion (orthotopic neobladder or continent catheterizable pouch), which is the preferred approach in appropriate candidates to best preserve and maintain quality of life. Further, receipt of neoadjuvant chemotherapy (systemic treatment administered before surgical resection), which has a proven survival benefit in combination with surgical therapy, should not be a deterrent to a minimally invasive strategy.
Similar to any complex cancer operation, the keys to a successful surgical outcome are the experience of the multi-disciplinary treatment team and a motivated patient. Technology should never trump practice, and optimal management of muscle invasive bladder cancer is best achieved at comprehensive, tertiary care centers that have performed a significant number of these procedures, open or robotic. However, in experienced hands, the benefits of a minimally invasive approach translate into a more rapid return to the normal activities of everyday life, which is an important goal for every patient.
Studies:
1.Parekh DJ, Messer J, Fitzgerald J, Ercole B, Svatek R. Perioperative outcomes and oncologic efficacy from a pilot prospective randomized clinical trial of open versus robotic assisted radical cystectomy. J Urol. 2013 Feb;189(2):474-9. doi: 10.1016/j.juro.2012.09.077. Epub 2012 Sep 24.
2. Nix J, Smith A, Kurpad R, Nielsen ME, Wallen EM, Pruthi RS. Prospective randomized controlled trial of robotic versus open radical cystectomy for bladder cancer. perioperative and pathologic results. Eur Urol. 2010 Feb;57(2):196-201. doi: 10.1016/j.eururo.2009.10.024. Epub 2009 Oct 20.
